The most dangerous pandemic to strike the world since the 1918 influenza outbreak, the coronavirus known as COVID-19, may have catastrophic effects on the U.S. health care system, our population and the economy.
There are few knowns, as the pandemic has not yet reached its peak and won’t for months. But new research by Andrew G. Atkeson, a consultant to the Federal Reserve Bank of Minneapolis, gives a basic model for economists and policymakers to use when projecting the economic consequences of COVID-19 progression scenarios.
According to the Minneapolis Fed: “The model focuses on the economic trade-off between disease progression and disease suppression through social distancing, focusing particular attention on the economic impact once active infection exceeds one percent of the U.S. population and 10 percent , as well as 18-month cumulative consequences.”
Atkeson draws several conclusions by using a SIR model of the progression of the disease over the next 12-18 months.
A SIR model is one of the simplest compartmental models, a technique used to simplify the mathematical modeling of infectious disease, with S standing for the number susceptible, I for the number of infectious and Rfor the number of recovered, deceased or immune individuals. The model has been proven to be reasonably predictive for a number of infectious diseases transmitted from human to human with recovery conveying lasting resistance.
How an epidemic plays out over time is determined by the transition rates between the three states. These transition rates are determined by characteristics of the underlying disease and by the extent of mitigation and social distancing measures imposed.
Even putting aside concerns about public health, it appears that there is a significant economic tradeoff whether or not we impose social distancing — the economic costs of strong social distancing measures imposed for an entire 12-18 months on the one hand or the economic costs of a large cumulative burden of lost work time.
The main conclusion is that even putting aside concerns about public health, the model predicts significant economic tradeoff whether or not we impose social distancing.
Even under severe social distancing scenarios, it is likely that the health system will be overwhelmed, which is indicated to happen when the portion of the U.S. population actively infected and suffering from the disease reaches one percent or about 3.3 million current cases.
More severe mitigation efforts push the date at which this happens back from six months from now to 12 months from now or more, perhaps allowing time to invest heavily in the resources needed to care for the sick. It’s clear that to avoid a health care catastrophe as is currently being experienced in Italy, prolonged severe social distancing measures will need to be combined with a massive investment in health care capacity.
The graph below plots the corresponding paths for cumulative cases and actively infected as a fraction of the population over the 18 months. The results of this simulation show remarkably small benefits to speedy application of mitigation measures in terms of reducing the peak fraction of the population infected. The primary benefit of speedy mitigation appears to be in delaying that period of peak infection.
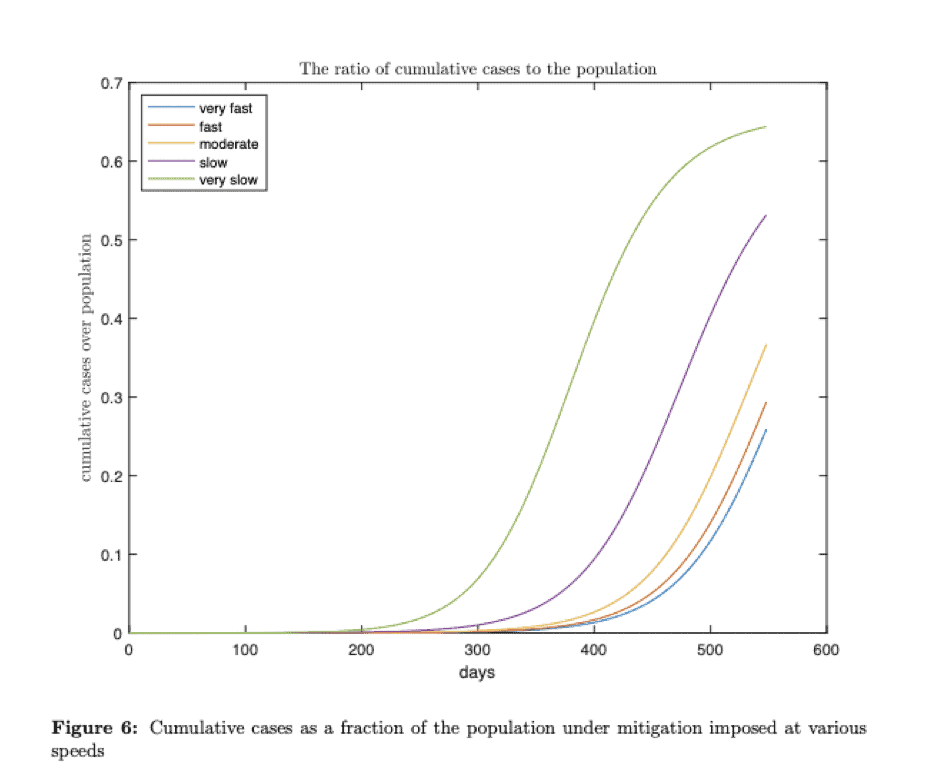
Under almost all of the scenarios considered, at the peak of the disease progression, between 10 percent and 20 percent of the population, a range of 33 to 66 million people, will suffer from an active infection at the same time. This level of infection in the population will likely require a significant diversion of the workforce from work to either self-quarantine and recuperation or caring for these sick individuals for a period of weeks or more.
It is also likely that all of this would have to occur without adequate support from the health care system for those with dire cases of the disease even if we implement a large investment in healthcare. In the model simulations, this peak infection period occurs between 7-14 months from now. It is imperative to try to understand how critical healthcare, economic, and financial infrastructure would function in a period of such concentrated disease burden should this come to pass.
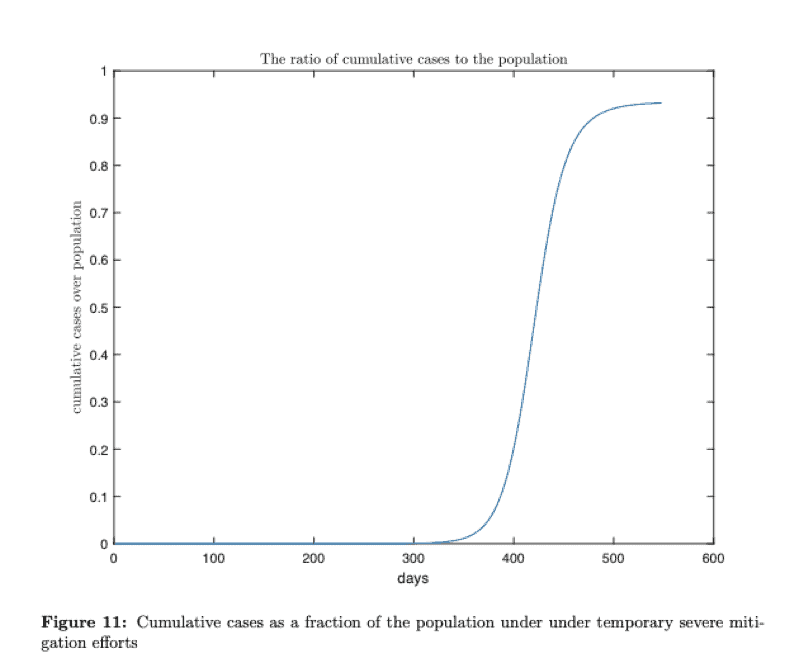
Several of the countries that experienced the disease early, including China, are relaxing the most severe mitigation efforts, Atkeson advises the move is unwise. Atkesons’s model, as demonstrated in the graph below, predicts that once mitigation efforts are relaxed, the disease simply restarts its rapid progression early in the second year.
Under those circumstances, COVD-19 reaches its peak infection rate about 450 days from now. A sustained mitigation effort will be required to capitalize on this success on early and short-term efforts.
The conclusions from Atkeson’s simple model are in line with those of the much more complex models that have been used by epidemiologists in advising governors, the president, and U.K. policymakers on emergency public health measures imposed over recent weeks.
Atkeson urges careful analysis of economic consequences of current mitigation steps “so that the economic trade-offs between public health and the economy can be considered quantitatively.” This will require open discussion between economists and public health experts, and between economic policymakers and the public.
SOURCE
https://www.minneapolisfed.org/article/2020/estimating-economic-impact-of-covid-19
